Researchers from the University of Vermont discuss their study, published by Oncotarget in 2017, titled, “Development of a predictive miRNA signature for breast cancer risk among high-risk women.”

The Behind the Study series transcribes videos of researchers elaborating on their papers published in Oncotarget. Visit the Oncotarget YouTube channel for more insights from outstanding authors.
—
Dr. Marie Wood
Hi, I’m Marie Wood. I’m at the University of Vermont. I’m a professor of medicine and I represent the clinical part of this program.
We created it back in 2003, a database prospectively gathered of women at increased risk for breast cancer. And it’s from that database that we took cases, and controls, and samples from women far prior to developing cancer.
Our goal was to see if we could really investigate these serum samples and their micro RNA profile, to see if we could come up with a profile of risk so that women might benefit in the long run by having a signal in their serum, a liquid biopsy if you will, to determine what is their risk of developing breast cancer years prior to developing it. I’d like to introduce my colleague Jane Lian.
Jane Lian
Hi, I’m the basic science part of this program. I’m a professor of biochemistry and we moved our whole lab to the University of Vermont in 2012, when I first met Dr. Wood. And the research background was our interest in identifying numerous micro RNAs that we had characterized as being drivers of tumor progression and metastatic bone disease, and actually in both breast and prostate cancer. But with Marie’s database offered, and just a wonderful opportunity to do longitudinal studies characterizing micro RNAs, that the literature and our laboratory that identify as being directly related to very specific cancer related events. So regular RNAs that marked the early/mid-stage and actual cancer aggressiveness, for the first time we could now look at women that were at risk, and we had just a very small percentage of boys, large database actually developed cancer. And so we could actually go back and compare those who got cancer to those who were still cancer free or at risk.
And by joining that, we came up with a signature of micro RNAs that could actually stratify these women into a risk category. And at this point, I would like to introduce Nick Farina, who joined our lab as a postdoctoral fellow. And he was actually the driver at the bench who developed all of the important protocols for going through all the data acquisition, including a very rigorous protocol for actually collecting the serum samples and analyzing them so that we would get very strong reproducibility and accuracy. And I am going to let Nicholas speak.
Nicholas Farina
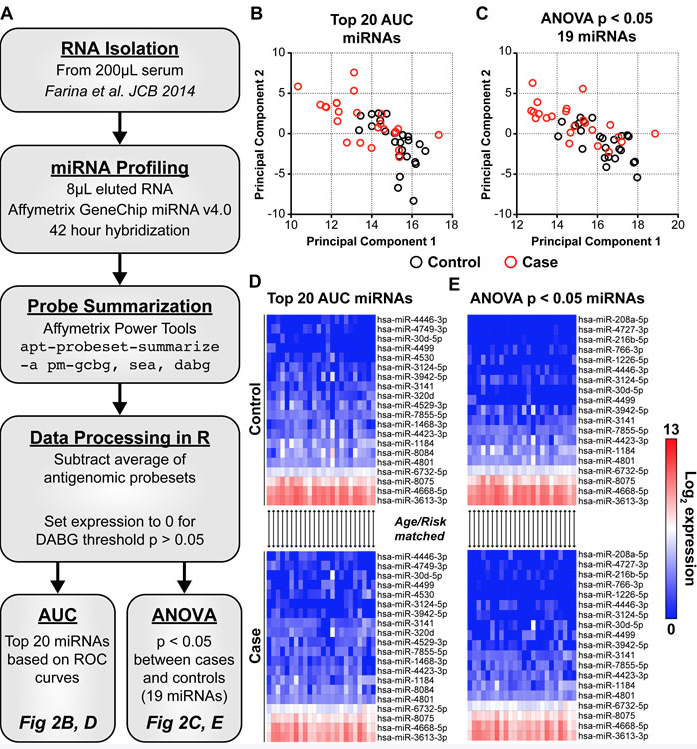
Hi. As Jane said, when I joined the lab, it was right shortly after they moved y’all from UMass and I met Dr. Wood with her pretty cool sample database that allowed us to actually ask if you identify risk marker for patients who well before they actually develop breast cancer. And so the first thing was to actually standardize both the isolation of RNA from serum.
I know that there has been a fair amount of work over the past many years by this was three or four years ago, I believe, when we first started to standardize the isolation protocol so we could reproducibly, consistently get good quality RNA. And then it was right around the time Admetrics updated the micro RNA array to the mere base version 20, that included an extra three to 400 micro RNAs used that were not available on the prior chips. And there’s also a slight difference in their chemistry. So the chips are more robust now. the screen was then to do the micro RNA profile on these women who are at risk and then went on to develop breast cancer, or that today remain cancer free. And we got all these profiles and didn’t really know what to do. We worked with the bioinformatics cohort here to develop an iterative stepwise model to identify those micro RNAs that best distinguish those women eventually being diagnosed breast cancer versus those that remained cancer-free.
And so had been a very joint and collaborative project between the hospital and the cancer center and the various cohorts. And then with that, I would like to introduce Dr. Gary Stein, the director of the cancer center
Dr. Gary Stein
And a long time friend and collaborator of these folks. So to me was is really important is it’s truthful. At the very general level of how we address the cancer problem, prevention becomes more important than ever before unquestionably. Prevention, early detection, if you have detectable disease, the earlier you detect it the treatment discussion should be far less detrimental to the patient and far more supportive, because quality of life becomes very key and cancer is becoming a preventable and treatable disease, but you need information. And if you can secure information through liquid biopsy, maybe a very small blood sample, then you have options that we can act on immediately.
And that’s going to expand as a function of time. This group has been focusing on non-coding RNAs. Micro RNAs are one dimensions of a problem, fragments and transfer RNAs are a second dimension of a problem. The problem all non-coding RNA’s are a dimension to the problem. And those dimensions are increasing very, very rapidly. So to us, this is very informative platform for decision-making and it is going to go ahead and be interfaced with a lot of initial information that was secure from the very, very same samples. And that is going to facilitate this objective of making cancer a preventable and treatable disease.
And the last point I was going to make is we want to be able to understand the earliest warning side, but we also want to be able to make the decision whether to treat or to continue to observe. And this information is going to contribute towards that type of decision-making as well.
Jane Lian
I was going to say we were very pleased with the response of the reviewers when we submitted our manuscript to Oncotarget and they really did appreciate the fact that, even though we had a small number of patients that would derive this information, it was something that was so useful for a physician and others who had similar types of databases to use these markers and validate what we had. And that’s really the long range goal. Is to make this an easy diagnostic set of parameters for evaluating risk.
Dr. Marie Wood
I wanted to make two points. One, the importance of a collaborative group of individuals who really listen to each other, but coming from very different backgrounds, it’s often very difficult for the basic science to listen to the clinical language. And we had some trials getting people to understand risk for cancer versus early detection, which this is not. This is risk for cancer years prior, it makes it very different. It doesn’t necessarily have implications on treatment because these biomarkers that we’ve identified and this profile is mirrors that haven’t really been described.
So it could be some environmental or genetic phenomenon that’s driving this risk, but that’s very different than prognostic markers. So that really sets this apart. current models that we have to assess women’s risk for cancer really fail us because they are going on the population level, but they’re not good on a personal level. So this, we hope, represents a jump forward for precision medicine in the prevention route.
Jane Lian
That brings us to something that was very rewarding for us when we moved the lab here, and that was the culture here at the University of Vermont, I guess Vermont in general, everyone is so supportive of each other, very collaborative and the clinicians have a lot of patience, so we’ve learned a lot from each other. So this project is really culminated into a wonderful example of what could be done.
Dr. Marie Wood
It also highlights the training that we do here at the University of Vermont. So to be able to be a post-doc and contribute this significantly to a project, I think, represents the commitment that people have to a teaching role, that leads into a mentoring role.
Nicholas Farina
Is was very nice to come home. I grew up in Vermont. To come home to find not only an honest environment to work in, but the exact kind of projects I was very interested in doing.
Click here to read the full study published by Oncotarget.