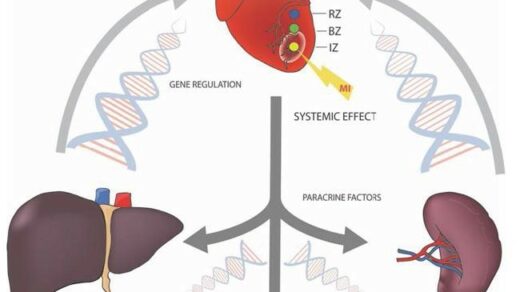
Researchers reveal their positive findings from a 2020 study on a strain of Salmonella typhimurium used in bacterial cancer therapy for mouse-modeled prostate cancer.
Over the past few decades, numerous studies have emerged using the promising strategy of bacteria as vehicles to deliver drugs or genes in tumor‐targeted therapies. Researchers say that bacterial cancer therapy may be able to overcome some of the limitations that conventional cancer therapy is stunted by, including the development of drug resistance.
In a 2020 study, researchers—from Yale University, the University of Missouri, Harry S. Truman Memorial Veterans Hospital, Cancer Research Center in Missouri, and DeSales University—investigated a tumor-targeting Salmonella typhimurium strain of bacteria (CRC2631) in prostate cancer-positive mouse-models and evaluated its toxicity, targeting ability and genetic stability. Their trending paper was published by Oncotarget and entitled, “Evaluations of CRC2631 toxicity, tumor colonization, and genetic stability in the TRAMP prostate cancer model.”
“Here, we report the toxicological and in vivo tumor-targeting profiles of CRC2631 in the syngeneic and autochthonous mouse model of aggressive prostate cancer, TRAMP (Transgenic Adenocarcinoma of Mouse Prostate).”
The Study
“To determine the safety profile of CRC2631, we performed CRC2631 and VNP20009 comparative toxicological studies in TRAMP animals.”
Two groups of 14-week-old B6FVB TRAMP-positive mice were treated with two methods of bacterial therapy; four mice were dosed with CRC2631, and four were dosed with VNP20009—one of the most studied tumor-targeting Salmonella enterica serovar Typhimurium strains—used here to compare CRC2631 safety. The team focused on measuring toxicity through treatment-related weight loss and lethality. For four weeks, both groups of mice were treated four times per week and monitored and weighed daily.
“VNP20009 is considered as the safety benchmark in bacterial cancer therapy development because it has been safely administered in human cancer patients [7, 30].”
The liver plays an important role in clearing bacteria from the bloodstream. Therefore, the researchers sought to establish the impact of this CRC2631 bacterial cancer therapy on liver pathology. Two groups of 31-week-old B6FVB TRAMP-positive mice were observed, one treated with four doses of CRC2631 and the other with saline (the control group) at three-day intervals. They used histological staining in the liver to observe differences in necrosis, inflammation and extramedullary hematopoiesis between CRC2631 and the control group.
Next, the team tested for lethality, maximum tolerated dose and the in vivo tumor-targeting capability of CRC2631 in the TRAMP mice. Using fluorescence imaging and a chloramphenicol resistance cassette, researchers were able to observe the biodistribution of CRC2631 to determine its tumor-targeting capability in TRAMP-positive mice. Since CRC2631 is filtered through the liver, enriched colonies may be found here. The researchers used the liver as a way to compare the bacterial load in tumor tissues.
CRC2631’s genetic stability was also tested by gauging its likelihood of regaining toxicity and/or losing tumor targeting capability by performing longitudinal, whole genome sequencing and short nucleotide polymorphism analyses. In vitro, CRC2631 directly kills prostate cancer cells, however, in vivo, CRC2631 does not lead to decreased tumor burden. The researchers believe this may be due to the effects of some kind of resistance mechanism in vivo. The team tested the effects of a combined treatment in their mouse models, using CRC2631 and Invivomab—a checkpoint blockade.
“CRC2631 targets and directly kills murine and human prostate cancer cells in vitro (Supplementary Figure 2), raising the possibility that unknown resistance mechanisms protect tumor cells from CRC2631-mediated cell death in vivo.”
Results
The researchers explained that within the first two weeks of the study, mice treated with CRC2631 and mice treated with VNP20009 both lost a comparable amount of weight. However, in the second half of the study, VNP20009-treated animals lost progressively more weight than those treated with CRC2631. This revealed that CRC2631 is less toxic than VNP20009.
“Consistent with CRC2631 being less toxic than VNP20009, the median survival time was 142 days for VNP20009 compared to 186 days for CRC2631 (Figure 1F).”
After evaluating effects in the liver from CRC2631, they found no differences in liver necrosis, inflammation or extramedullary hematopoiesis between mice in the CRC2631 treated group and the control group. CRC2631 did not cause overt liver pathology. The researchers established the maximum tolerated dose was two doses of five × 10^7 colony forming units, administered three days apart. In the model used in fluorescence imaging, they found that CRC2631 was significantly colonized in the tumor tissue of mice when compared to colonization in the liver and, as the dosage increased, CRC2631 quantities in tumor tissues also increased. These findings validated the primary tumor and metastases targeting capability of CRC2631.
The researchers determined CRC2631 to be a genetically stable tumor-targeting mechanism. They revealed that it would take approximately 9375 days for CRC2631 to acquire a potential mutation in any specific gene. Next, the researchers collected results from the CRC2631 and Invivomab immune checkpoint blockade combination.
“We turned our focus to an interaction between CRC2631 and immune cells and asked whether tumor-targeted CRC2631 generates an anti-tumor immune response that tumors rapidly inhibit via immune checkpoint mechanisms.”
They found that tumor burdens were significantly reduced in the combination treatment method, and ultimately, that CRC2631 treatment with a checkpoint blockade combination reduces the metastatic burden in mouse-modeled prostate cancer.
Conclusion
The study as a whole revealed that CRC2631 safely targets primary tumors and metastases, is less toxic than VNP20009, does not cause overt liver pathology and, in combination with an immune checkpoint blockade such as Invivomab, it reduces metastatic burden in vivo in B6FVB TRAMP-positive mice. With more research, this method may soon be studied as an effective clinical treatment option for human prostate cancer.
“These findings indicate that CRC2631 is a genetically stable biologic that safely targets tumors. Moreover, tumor-targeted CRC2631 induces anti-tumor immune activity and concordantly reduces metastasis burden in the setting of checkpoint blockade.”
Click here to read the full scientific study, published by Oncotarget.
YOU MAY ALSO LIKE: More Oncotarget Videos on LabTube
—
Oncotarget is a unique platform designed to house scientific studies in a journal format that is available for anyone to read—without a paywall making access more difficult. This means information that has the potential to benefit our societies from the inside out can be shared with friends, neighbors, colleagues and other researchers, far and wide.
For media inquiries, please contact media@impactjournals.com.